SPIRALING HIGH BLOOD PRESSURE LINKED TO NITRIC OXIDE DEFICIENCY
STUDY HELPS EXPLAIN WHY UNCONTROLLED BLOOD PRESSURE GETS WORSE; MAY POINT WAY TO MORE EFFECTIVE TREATMENTS
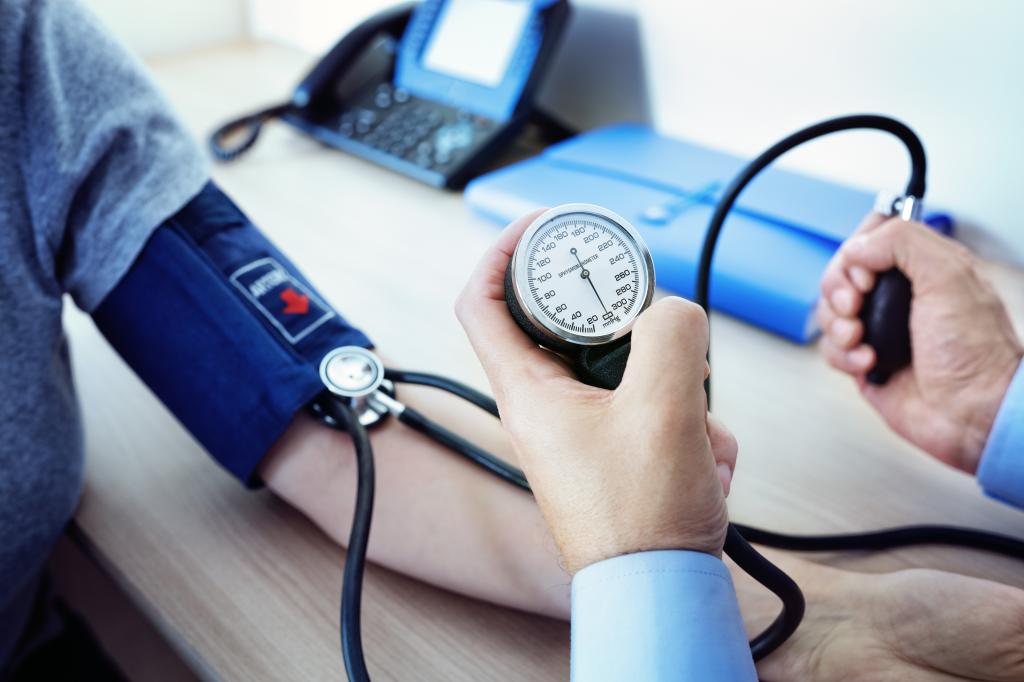

Irvine, Calif., Aug. 31, 2001 — When high blood pressure isn’t controlled, it doesn’t stay at one high level. Instead, it spirals higher and higher, greatly increasing the risk of heart attack and stroke.
According to a UC Irvine College of Medicine study, this pattern occurs because high blood pressure causes the inactivation of nitric oxide, an important molecular regulator of blood pressure. This inactivation then triggers a vicious circle of increased nitric oxide inactivation and ever higher, uncontrolled blood pressure.
The study is believed to be the first to show how this inactivation can lead to spiraling blood pressure and may lead scientists to develop more effective ways to control high blood pressure. It appears in the September 2001 issue of Kidney International.
The study, conducted on rats by Dr. Nick Vaziri, professor of medicine and chief of nephrology, and his colleagues, found that nitric oxide, which helps control blood pressure by dilating blood vessels, is inactivated by increasing blood pressure. As pressure increases, molecules called free radicals and reactive oxygen species cause cellular damage and inactivate nitric oxide, causing blood pressure to keep rising. As blood pressure continues to rise, more nitric oxide is inactivated, causing pressure to rise even higher.
“This vicious circle of high blood pressure, nitric oxide inactivation and subsequently higher pressure shows us that a rise in blood pressure alone can increase free radicals, which inactivate nitric oxide and raise blood pressure further,” Vaziri said. “While the initial causes of high blood pressure are diverse and in many cases unclear, this study shows the importance of making sure high blood pressure is always controlled and may provide greater understanding of how to better do so.”
High blood pressure affects more than 25 million Americans and is a major risk factor for heart disease and stroke. The American Heart Association estimates that less than one-third of people with high blood pressure control it effectively.
Vaziri and his colleagues showed previously that increased free radical activity plays an important role in all cases of high blood pressure. They further showed that increased levels of free radicals by themselves can cause hypertension. Harmful levels of free radicals are often reduced by certain antioxidants, including Vitamin E and other chemicals found in food.
In this study, the researchers asked whether hypertension itself can increase this free radical production, using rats that had high blood pressure in the front half of the body and normal pressure in the rear half.
The rats’ front halves showed significant increases in a chemical called nitrotyrosine, a product of nitric oxide inactivation by reactive oxygen species. In the rats’ rear halves (which had normal blood pressure), no significant increases of this chemical were found, indicating normal levels of free radicals. The researchers concluded that pressure was regulating the amount of free radicals in the body, which inactivated nitric oxide and created the cycle of pressure, leading to cardiovascular and kidney diseases.
“Nitric oxide inactivation was seen in restricted arteries with high pressure but not in open arteries. This indicates that this circle of inactivation and pressure is made worse by the mechanical pressure and not by genetic or hormonal interactions affecting the body as a whole,” Vaziri said. “Free radicals and other such molecules, then, play a much stronger role in high blood pressure than has been previously assumed. These molecules may hold the key to controlling excessively high pressure and perhaps to better treatments using antioxidants and other chemicals to keep pressure normal.”
Vaziri and his colleagues have been focusing for years on the complex chemical interactions that lead to high blood pressure. They now are working on a number of experiments to better define the relationships between blood pressure, nitric oxide and the risk of disease in the kidney, heart and brain. Vaziri’s colleagues in the study include Drs. Cyril Barton and Zhemin Ni of UCI.
Media Contact:
Andrew Porterfield
(949) 824.3969
amporter@uci.edu
Kim Pine
(714) 456-7759
kpine@uci.edu
